Abstract
Introduction
Resistance to eye opening (REO) is a commonly encountered phenomenon in clinical practice. We aim to investigate whether REO is a sign of consciousness or a reflex in severely brain-injured patients.
Methods
We recorded REO in chronic patients with disorders of consciousness during a multimodal diagnostic assessment. REO evaluations were performed daily in each patient and clinical diagnosis of unresponsive wakefulness syndrome (UWS), minimally conscious state with (MCS+) or without (MCS−) preserved language processing was made using the Coma Recovery Scale-Revised (CRS-R).
Results
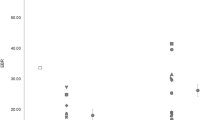
Out of 150 consecutive patients, 79 patients fit inclusion criteria. REO was seen in 19 patients (24.1%). At the group level, there was a significant relationship between the presence of REO and the level of consciousness. We also observed a difference in the repeatability of REO between patients in UWS, MCS− and MCS+. Out of 23 patients in UWS, six showed REO, in whom five showed atypical brain patterns activation.
Conclusion
Our findings suggest a voluntary basis for REO and stress the need for multiple serial assessments of REO in these patients, especially since most patients show fluctuating levels of consciousness.


Similar content being viewed by others
References
Miller Fisher C (1963) Reflex blepharospasm. Neurology 13:77. https://doi.org/10.1212/WNL.13.1.77
DeToledo JC, Ramsay RE (1996) Patterns of involvement of facial muscles during epileptic and nonepileptic events: review of 654 events. Neurology 47:621–625. https://doi.org/10.1212/WNL.47.3.621
Young JL, Rund D (2010) Psychiatric considerations in patients with decreased levels of consciousness. Emerg Med Clin North Am 28:595–609. https://doi.org/10.1016/j.emc.2010.03.010
Hurwitz TA (2011) Psychogenic unresponsiveness. Neurol Clin 29:995–1006. https://doi.org/10.1016/j.ncl.2011.07.006
Larumbe R, Vaamonde J, Artieda J, Zubieta JL, Obeso JA (1993) Reflex blepharospasm associated with bilateral basal ganglia lesion. Mov Disord 8:198–200. https://doi.org/10.1002/mds.870080215
Grandas F, López-Manzanares L, Traba A (2004) Transient blepharospasm secondary to unilateral striatal infarction. Mov Disord 19:1100–1102. https://doi.org/10.1002/mds.20109
Jankovic J, Patel SC (1983) Blepharospasm associated with brainstem lesions. Neurology 33:1237. https://doi.org/10.1212/WNL.33.9.1237
Iizuka T, Sakai F, Ide T, Monzen T, Yoshii S, Iigaya M, Suzuki K, Lynch DR, Suzuki N, Hata T, Dalmau J (2008) Anti-NMDA receptor encephalitis in Japan: long-term outcome without tumor removal. Neurology 70:504–511. https://doi.org/10.1212/01.wnl.0000278388.90370.c3
Choe CH, Gausas RE (2012) Blepharospasm and apraxia of eyelid opening associated with anti-Hu paraneoplastic antibodies: a case report. Ophthalmology 119:865–868. https://doi.org/10.1016/j.ophtha.2011.10.008
Minkowski M (1921) Sur les mouvements, les reflexes, et les reactions musculaires du foetus humain de 2 a 5 mois et leurs relations avec le systeme nerveux foetal. Rev Neurol (Paris) 37:1105
Deuschl G, Goddemeier C (1998) Spontaneous and reflex activity of facial muscles in dystonia, Parkinson’s disease, and in normal subjects. J Neurol Neurosurg Psychiatry 64:320–324. https://doi.org/10.1136/jnnp.64.3.320
Pearce J, Aziz H, Gallagher JC (1968) Primitive reflex activity in primary and symptomatic Parkinsonism. J Neurol Neurosurg Psychiatry 31:501–508
Laureys S, Celesia GG, Cohadon F, Lavrijsen J, León-Carrión J, Sannita WG, Sazbon L, Schmutzhard E, von Wild KR, Zeman A, Dolce G (2010) Unresponsive wakefulness syndrome: a new name for the vegetative state or apallic syndrome. BMC Med 8:68. https://doi.org/10.1186/1741-7015-8-68
Giacino JT, Ashwal S, Childs N, Cranford R, Jennett B, Katz DI, Kelly JP, Rosenberg JH, Whyte J, Zafonte RD, Zasler ND (2002) The minimally conscious state: definition and diagnostic criteria. Neurology 58:349–353
Bruno M-A, Vanhaudenhuyse A, Thibaut A, Moonen G, Laureys S (2011) From unresponsive wakefulness to minimally conscious PLUS and functional locked-in syndromes: recent advances in our understanding of disorders of consciousness. J Neurol 258:1373–1384. https://doi.org/10.1007/s00415-011-6114-x
Gosseries O, Di H, Laureys S, Boly M (2014) Measuring consciousness in severely damaged brains. Annu Rev Neurosci 37:457–478. https://doi.org/10.1146/annurev-neuro-062012-170339
Seel RT, Sherer M, Whyte J, Katz DI, Giacino JT, Rosenbaum AM, Hammond FM, Kalmar K, Pape TL-B, Zafonte R, Biester RC, Kaelin D, Kean J, Zasler N (2010) Assessment scales for disorders of consciousness: evidence-based recommendations for clinical practice and research. Arch Phys Med Rehabil 91:1795–1813. https://doi.org/10.1016/j.apmr.2010.07.218
Bodart O, Gosseries O, Wannez S, Thibaut A, Annen J, Boly M, Rosanova M, Casali AG, Casarotto S, Tononi G, Massimini M, Laureys S (2017) Measures of metabolism and complexity in the brain of patients with disorders of consciousness. NeuroImage Clin 14:354–362. https://doi.org/10.1016/j.nicl.2017.02.002
Stender J, Gosseries O, Bruno M-A, Charland-Verville V, Vanhaudenhuyse A, Demertzi A, Chatelle C, Thonnard M, Thibaut A, Heine L, Soddu A, Boly M, Schnakers C, Gjedde A, Laureys S (2014) Diagnostic precision of PET imaging and functional MRI in disorders of consciousness: a clinical validation study. Lancet (Lond, Engl) 384:514–522. https://doi.org/10.1016/s0140-6736(14)60042-8
Monti MM, Vanhaudenhuyse A, Coleman MR, Boly M, Pickard JD, Tshibanda L, Owen AM, Laureys S (2010) Willful modulation of brain activity in disorders of consciousness. N Engl J Med 362:579–589. https://doi.org/10.1056/NEJMoa0905370
Schiff ND (2015) Cognitive motor dissociation following severe brain injuries. JAMA Neurol 72:1413–1415. https://doi.org/10.1001/jamaneurol.2015.2899
Posner JB, Saper CB, Schiff ND, Plum F (2007) Plum and Posner’s diagnosis of stupor and coma, 4th edn. Oxford University Press, New York
Gosseries O, Zasler ND, Laureys S (2014) Recent advances in disorders of consciousness: focus on the diagnosis. Brain Inj 28:1141–1150. https://doi.org/10.3109/02699052.2014.920522
Kato M, Miyauchi S (2003) Functional MRI of brain activation evoked by intentional eye blinking. Neuroimage 18:749–759. https://doi.org/10.1016/S1053-8119(03)00005-3
Acknowledgements
The study was supported by the University and University Hospital of Liège, the Belgian National Funds for Scientific Research (FRS-FNRS), Human Brain Project (EU-H2020-fetflagship-hbp-sga1-ga720270), Luminous project (EU-H2020-fetopen-ga686764), the French Speaking Community Concerted Research Action (ARC-06/11-340), the James McDonnell Foundation, Mind Science Foundation, IAP research network P7/06 of the Belgian Government (Belgian Science Policy), the European Commission, the Public Utility Foundation ‘Université Européenne du Travail’, “Fondazione Europea di Ricerca Biomedica”, and the BIAL Foundation. OB is a research fellow, AT, VCV and OG are post-doctoral fellows, and SL is research director at FRS-FNRS. The authors thank Prof. Pierre Maquet from the Neurology department, University Hospital of Liège, as well as the whole Neurology staff, patients and their families.
Author information
Authors and Affiliations
Contributions
The authors have contributed to conception and design of the study (HJvO, SL, OG), acquisition and analysis of data (HJvO, AT, AV, LH, VCV, SW, OB, OG), writing of the manuscript (HJvO, OG), creation of the figures (HJvO, OG) and critical revision of the manuscript for intellectual content (AT, AV, LH, VCV, SW, OB, SL).
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical standards
The study was approved by the Ethics Committee of the Medical School of the University of Liège and written consents were obtained from the legal representative of each patient.
Rights and permissions
About this article
Cite this article
van Ommen, H.J., Thibaut, A., Vanhaudenhuyse, A. et al. Resistance to eye opening in patients with disorders of consciousness. J Neurol 265, 1376–1380 (2018). https://doi.org/10.1007/s00415-018-8849-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-018-8849-0